Vaginal atrophy can cause considerable issues for postmenopausal women. This treatable condition can dramatically decrease the patient’s quality of life. It is estimated that only 25% of those who suffer from the condition will seek medical help. Primary care clinicians (PCP) should know about vaginal atrophy to respond quickly when patients present with possible symptoms.
1. Why primary care physicians should address vaginal atrophy
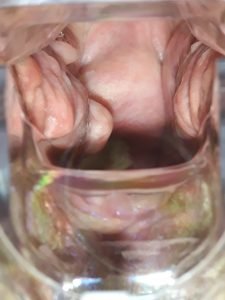
Vaginal atrophy is caused by decreasing levels of estrogen in menopausal women. Unlike hot flashes and night sweats that might resolve spontaneously over time, the effects on the vagina are often progressive. As time progresses increased dryness, lax vaginal walls and thinning vaginal tissue can cause itching, burning, dyspareunia and compromised sexual functioning.
Usually becoming clinically apparent 4-5 years after the onset of menopause, studies suggest that
25-50% of women experience vaginal atrophy.
 Only a quarter of those affected will seek medical treatment. One study found that 42% of women who did not seek medical treatment for their vaginal atrophy felt that it was unimportant. A further 13% thought it was ‘something to put up with’ and not deserving of medical attention. Sadly, 10% were too embarrassed to discuss the problem with their physician.
Only a quarter of those affected will seek medical treatment. One study found that 42% of women who did not seek medical treatment for their vaginal atrophy felt that it was unimportant. A further 13% thought it was ‘something to put up with’ and not deserving of medical attention. Sadly, 10% were too embarrassed to discuss the problem with their physician.
As the healthcare providers that patients interact with most frequently, primary care providers and family physicians have the opportunity to overcome some of these barriers. By being aware of the potential symptoms of vaginal atrophy and feeling empowered to ask patients about their experience, PCPs can help treat those patients who might otherwise suffer needlessly.
2. Causes of vaginal atrophy
 As menopause progresses, levels of estrogen decrease from 147 to 1468 pmol/l to less than 73 pmol/l. This drop in estrogen levels results in a change in vaginal physiology and relating symptoms.
As menopause progresses, levels of estrogen decrease from 147 to 1468 pmol/l to less than 73 pmol/l. This drop in estrogen levels results in a change in vaginal physiology and relating symptoms.
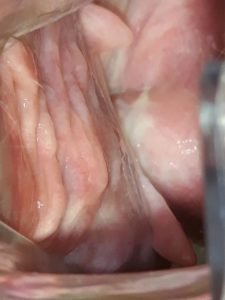
The reduction of estrogen production post menopause combines with the natural atrophy of the skin and mucosal surfaces, due to aging, causing vaginal atrophy. A breakdown of collagen support of the vaginal epithelium also causes loss of rugosity in the vaginal rugal folds which can contribute to vaginal prolapse.
The pH levels of the vagina increase in menopause, from <4.5 to over 6. This leaves the postmenopausal vagina at greater risk of infections and inflammation.
3. Possible symptoms
There are many symptoms that can indicate vaginal atrophy. Some are more common than others. In their Recommendations for the Management of Postmenopausal Vaginal Atrophy, the International Menopause Society suggests that the most common symptoms of vaginal atrophy include dryness (estimated at 75% of women), dyspareunia (estimated at 38%), and vaginal itching, discharge and pain (estimated at 15%).
Possible other symptoms of vaginal atrophy:
- Dryness and insufficient moistness
- Dyspareunia
- Itching
- Burning sensation
- Mucosal defects including petechiae, microfissures, ulceration, and inflammation
- Soreness
- Shortening, fibrosis, obliteration of vaginal vault and/or narrowing of the vaginal entrance
- Susceptibility to mechanical injuries
- Adverse impact on the healing of mechanical and postoperative wounds
4. How best to confer with expert gynecologists at the point of care
If a primary care physician is unsure about a potential case of vaginal atrophy, it is possible to receive professional support in their own clinic. Developments in telehealth now allow physicians at the point-of-care to share cases with colleagues. This enables a family doctor to receive immediate expert input for gynecologic cases, confirming a diagnosis, offering suggestions for treatment and advising when a referral is recommended.
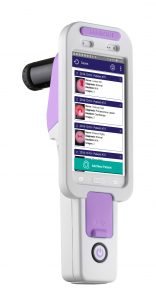 The EVA System is a complete visualization solution for vaginal, vulvar and cervical exams. Using the Teleconsultation feature, a physician at the point-of-care is able to securely share images and video with a remote colleague. The physicians can hear and see each other throughout the teleconsultation allowing for discussion and sharing of information.
The EVA System is a complete visualization solution for vaginal, vulvar and cervical exams. Using the Teleconsultation feature, a physician at the point-of-care is able to securely share images and video with a remote colleague. The physicians can hear and see each other throughout the teleconsultation allowing for discussion and sharing of information.
Teleconsultation provides a significant benefit to patients as it can reduce the need for external referrals, allowing patients to receive specialist care within their own familiar primary care practice, and reducing the need for additional appointments. Studies into teleconsultation for gynecologic procedures found that patients actually prefer teleconsultation as they are reassured by having an additional consulting physician.
Especially in cases such as vaginal atrophy, where patients might be unwilling to consult an unfamiliar physician, teleconsultation can help primary care physicians to provide their patients with an expert opinion.
5. Treatment options
There are a number of treatments that can be used to address vaginal atrophy. Some simply respond to the symptoms while others address the underlying causes. We spoke with Dr. Scott Eder MD, GYN, Center for Women’s Health & Wellness, Lawrenceville, NJ. Dr. Eder shared some of his preferred products in each category.
Lubricants
Lubricants can help to decrease discomfort during intercourse. There are significant differences between the many different lubricants available on the market, depending primarily on the osmolarity of the lubricant. There are times when the use of lubricants can be counter-productive as they might further reduce the levels of natural moisturization in the vagina. Dr. Eder adds, “It is important that patients be warned not to use Vaseline as an internal lubricant as it can break down the latex of condoms and cause vaginal irritation.”
Vaginal Moisturizers
Another topical solution with a longer-lasting effect than simple lubricants are vaginal moisturizers. These are hydrophilic, insoluble cross-linked polymers that are bio-adhesive. They attach to the mucin and epithelial cells on the vaginal wall retaining water. Dr. Eder typically prescribes Replens vaginal moisturizer to be applied twice weekly.
Vaginal Estrogens
Topical vaginal estrogens are one of the most popular vaginal atrophy treatments. It has proven effective in relieving symptoms without causing a proliferation of vaginal epithelium. As the genitourinary pH levels are lowered it also helps to decrease urinary tract infections. “Some women prefer a vaginal suppository, like Vagifem, to tropical creams,” suggests Dr. Eder.
Oral estrogen replacement
There are multiple benefits to oral estrogen replacement therapy for menopausal women. When administered at the onset of menopause it can even prevent the development of urogenital symptoms. As well as reducing the symptoms of vaginal atrophy, oral estrogen replacement has the additional benefit of decreasing postmenopausal bone loss and alleviation of vasomotor dysfunction. Some women may require coadministration of topical vaginal estrogen.
Non-hormone based treatments: Vaginal Inserts
Dr. Eder has some patients that prefer to pursue a non-hormone based treatment. He explains, “There was some debate in the press suggesting that hormone replacement therapy increased risk of heart attack and cancer. This has now been mostly debunked but some patients are still concerned.”
The vaginal insert Intrarosa uses the active ingredient prasterone, which is also known as dehydroepiandrosterone (DHEA), which is a successful alternative for many women.
Laser treatment
In some cases that fail treatment with estrogen replacement, either topical or oral, functional gynecology laser treatment has been shown to be a promising alternative. The procedure using a fractional co2 laser (such as Femtouch) drives increased blood flow to the vaginal tissue which alleviates the symptoms of vaginal atrophy.
By arming themselves with both the necessary background information and the practical tools needed to confer when necessary, family and primary care physicians are able to provide their patients with thorough treatment for vaginal atrophy and related conditions.







