Diethylstilbestrol (DES) was marketed to prevent miscarriage, premature labor and other pregnancy-related complications from 1940 to 1971. However, this synthetic form of estrogen caused significant birth defects, notably leaving children born to the mother who had taken DES with structural abnormalities in the genital tract and at an increased risk of related cancers.
Dr. Mary Rubin, PhD, NP, coordinated the University of Pennsylvania DES center for twenty years, giving her a unique insight into this population. She shares her experience:
 DES was initially synthesized in England in 1938 as a treatment for preventing miscarriage early in pregnancy. It was later used for women who were diabetic or had suffered a miscarriage, had blood incompatibility or had other pregnancy complications. Although later research showed that DES did not have any real clinical benefit for minimizing pregnancy complications, the medical community embraced this “new miracle drug” and used it regularly for an extended period of time.
DES was initially synthesized in England in 1938 as a treatment for preventing miscarriage early in pregnancy. It was later used for women who were diabetic or had suffered a miscarriage, had blood incompatibility or had other pregnancy complications. Although later research showed that DES did not have any real clinical benefit for minimizing pregnancy complications, the medical community embraced this “new miracle drug” and used it regularly for an extended period of time.
The effects of Diethylstilbestrol (DES)
DES was found to be a teratogen and carcinogen, which caused serious birth defects when taken in the first trimester of pregnancy during the formation of the fetal genitalia.
Close to 10 million children and mothers were exposed to DES.
Both genders frequently showed unusual genital tract changes and structural variations. While the majority did not develop cancer, there was an increased risk of cervical cancer increased among the girls (1:1000-1:100,000). Some DES sons, as the boys were known, experienced hypospadias, low sperm count and later infertility. However, early data on DES sons was much more limited.
DES daughters had more pronounced structural variations in the genital tracts. Commonly found issues included:
- Cervical collar formation – an extra lip of tissue grew around the cervix.
- An enlarged transformation zone which increased the risk of cervical cancer as there were larger areas in which lesions could develop.
- Flattening of the cervix – instead of protruding into the vagina, the cervix was flattened upwards. This caused many issues in their own pregnancies as the cervix would open prematurely as the baby developed.
 Case Study 1
Case Study 1
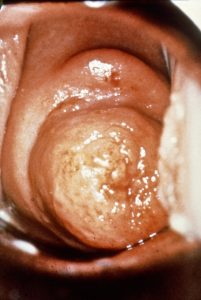
The cockscomb, collar, and pseudopolyp of the cervix. Cockscomb (hoods) are markedly enlarged folds of cervical stroma and epithelium. Low, broad folds are collars (rims). A pseudopolyp is that portion of the cervix which is medial to a constricting band (sulcus) and has on a superficial examination of the appearance of a polyp. However, the pseudopolyp is not a true polyp since the endocervical canal transverses through it.
The creation of the DES Center
There were a high number of DES children born in the Philadelphia area, party due to one particular OB-GYN practice prescribing it to all their pregnant patients. The DES Center at the University of Pennsylvania was created to evaluate these and other DES patients and study their progress to better understand the effects of the drug. Once that particular practice ceased to be in operation, the DES Center was able to access their records and began systematically reaching out to past patients to place DES children under ongoing observation.
Susan* was one such mother. She’d already experienced two miscarriages and hoped to carry her third pregnancy to term. Therefore, her OB-GYN prescribed DES right after confirming the pregnancy. When the DES Center contacted Susan to explain the risks that were posed to her daughter, Lucy*, she immediately scheduled an appointment for screening.
The screening with all patients started with palpating the vagina for nodularity before performing a Pap test. Then patients would receive a visual screening with colposcopy to determine whether any unusual tissue appeared precancerous or cancerous. Performing colposcopy and biopsies was no simple matter, especially in the 1970’s.
A large percentage of the DES children were in their early teens, with some as young as seven. Such young patients were afraid of the procedure. From a physical perspective, inserting a speculum was challenging. For a few patients, it was impossible to perform colposcopy in the outpatient setting, and it became necessary to perform the exam after putting the patient under anesthesia. Even after every attempt to make the experience as acceptable as possible, many developed very negative associations with the procedure that caused loss-to-follow-up issues.
*Names have been changed
Performing colposcopy on young girls
As Lucy was only eight when she came for her first screening, I recommended that Susan help her to first insert a small tampon and then gradually increase the size to accustom her to the process of having something inserted into her vaginal canal. Although still a trying experience at such a young age, this gave her some familiarity with the sensations involved. The DES Action group already had chapters in several areas of the country including the University of Pennsylvania. Mothers and daughters were encouraged to attend meetings and share experiences in coping with this diagnosis and the necessary steps to monitor their health.
While most of the DES daughters did not develop cervical cancer, they were all advised to undergo annual check-ups instead of following the standard recommendation of cervical cancer screening every three years. Many of the structural changes self-corrected as time went on. The long-term need for colposcopic evaluation depends on maintaining normal cytology and normal development of the transformation zone. The time frame for this process varies from patient to patient and is influenced by many factors.
 Case Study 2
Case Study 2
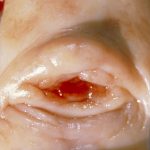
Hypoplastic cervix in which there is a cockscomb anteriorly and collar posteriorly.
DES daughters in adulthood and beyond
As DES daughters reached their own childbearing years, many experienced miscarriage and difficulties in pregnancy. Others had no problems while experiencing multiple successful pregnancies. While it is likely that the pregnancy difficulty was due to the effects of DES exposure, the fact that they were coming from families with a history of pregnancy difficulties needs to be factored into the explanation for some of the morbidity.
Thankfully, no known difficulties transferred to the second generation. Lucy was such an example. Having undergone colposcopy in her childhood, she developed a strong aversion to the procedure. Despite being strongly advised to continue annual screenings, she went six years before deciding that her health was more important than the discomfort of colposcopy. Thankfully, she had not developed any symptoms in the interim years. For some DES daughters, only when problems presented themselves did they return for evaluation and treatment. Also, when something appeared in the news about DES exposure, that triggered a return visit.
Most of the patients treated by the DES Center did maintain their screening schedule, helping to contain the potential rise in related cervical cancer cases. The care and the support they received from their clinicians helped to create strong bonds that reassured they were in good hands while they matured into young adults.
Now, as DES daughters such as Lucy reach their senior years, continued monitoring is necessary. Healthcare providers must educate their patients that, although most DES daughters have reached menopause and many normal physical changes have already taken place, we do not know for certain what the future may hold.
DES resources
About the author:

Mary Rubin, BSN, MSN, PhD
Mary Rubin, BSN, MSN, PhD University of Pennsylvania, Clinical Professor of OB-GYN UCSF, has spent over 45 years as a clinician, educator and researcher. She pioneered the role of a nurse colposcopist. Having held faulty positions in multiple programs, including ASCCP, HIS, Harbor UCLA, and PPFA, Mary Rubin was the first nurse practitioner on the ASCCP board of directors. She received the ASCCP Lifetime Achievement Award.







