A recent Twitter feud has brought to the light the pervasive misconceptions about the female body. Many women do not know the difference between the terms vagina and vulva. This lack of patient understanding can have an impact on healthcare outcomes.
In February 2019, The Guardian published an excerpt from an upcoming book, Womanhood: The Bare Reality by the photographer and writer, Laura Dodsworth. The work features a collection of photographs of the vulva along with first-person testimonials.
When the Guardian posted the article on Twitter, a man responded to the Tweet, “The correct word is vagina.” The comment sparked a wave of backlash defining the difference between vagina and vulva.
The correct word is vagina.
— Herr Doktor Bullen (Paul) (@paulbullen) February 10, 2019
“I am supporting widespread female usage, as in The Vagina Monologues,” the man contended. “I am defending how actual people speak.”
The discussion highlights an important problem: The word vagina is regularly misused. A survey of 1,000 British women demonstrated that 44 percent could not correctly identify the vagina on a medical illustration of the female reproductive tract. Even fewer could recognize the vulva (60 percent of participants failed at this task).
In an interview, Tracie Miles, nurse at Eve Appeal explained, “The lack of basic knowledge about the female body is extremely worrying. How can we expect women to know what to look out for in terms of unexpected changes in their vagina or vulva, or to be aware of the signs and symptoms of a gynecological cancer if they’re not body-aware?”
Misconceptions of the female anatomy have repercussions in health and treatment
Misconceptions of vaginal health begin at an early age. Adolescent females have very specific views about their vaginas and lack a clear understanding of what constitutes normalcy of the vagina and future fertility as well as how to make safe and appropriate choices about their bodies.
Vaginal narratives, influenced by sexism, racism, and homophobia, negatively impact female body image, grooming, and health habits. A study of adult women, age 34 on average, used strong language such as “dirty”, “gross”, “needing maintenance”, or “unnatural” when speaking about their genitals, evoking emotions of “anxiety, excess, and the need for control”.
This shameful attitude may also interfere with a woman’s ability to speak openly about health concerns with a doctor.
Women in menopause, who do not have adequate knowledge of changes in their vaginal health, avoid consulting any healthcare professional when they should proactively initiate discussions on appropriate treatments, according to a survey conducted in the United States.
How much does it matter if patients don’t understand their anatomy?
One might think that a lack of patient understanding about the vagina and vulva is not critical. However, using incorrect terminology to describe symptoms can interfere with a physician’s ability to provide prompt diagnosis and treatment.
“If your patient says that their vagina itches, when they really mean vulva, then you can waste time getting them to clarify so you can make sure they receive the correct treatment,” warns Dr. Jonah Mink, Medical Director at MobileODT.

Patient understanding improves medical outcomes
A multitude of studies conclude that patient understanding improves medical outcomes across specialties. Patients, empowered with the knowledge of their own bodies and treatment, repeatedly show greater health and clinical outcomes, including better disease management, more effective use of healthcare, improved health condition and medication adherence. Specifically in obstetrics and gynecology, educating patients about their anatomy and necessary procedures has shown proven success in treatment.
Educating women about their bodies starting at a young age can help to teach about the normalcy of the female reproductive system and promote healthy behaviors.
Teaching women about their health encourages them to receive regular exams, seek treatment when experiencing abnormal symptoms, and empower them with the vocabulary to describe their own bodies and health status. Patient education can also help dispel myths and misconceptions about the female anatomy.

How to educate patients by showing them their own anatomy
Physicians can improve patient understanding through a number of recommended approaches including printed materials such as handouts, audio-visual methods, demonstrations, and verbal instructions.
In addition to the misconceptions of the female anatomy, more complex medical terminology poses a challenge as many words that describe conditions and treatments are long and multisyllabic with no short synonyms. Physicians can supplement verbal descriptions with visual tools like images and video to clarify any potential confusion or preconceived misconceptions.
The EVA WELL System, for example, provides a powerful tool for teaching women about their anatomy and treatments at the point of care. During gynecologic exams, EVA WELL allows physicians to show patients images and video on a screen in real-time.
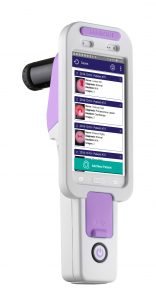 After the exam, the physician can email images to patients for their own peace of mind. Pablo Naranjo, MD at Nisa Hospital Madrid, writes of his experience using visual tools to teach patients,“ With EVA Well, my patients are engaged throughout their treatment. I can even email them the images afterward.”
After the exam, the physician can email images to patients for their own peace of mind. Pablo Naranjo, MD at Nisa Hospital Madrid, writes of his experience using visual tools to teach patients,“ With EVA Well, my patients are engaged throughout their treatment. I can even email them the images afterward.”
This example of patient engagement in the medical process helps to “cultivate patients’ confidence” as patients will “directly benefit from health gains of being activated and empowered.” Patients benefit from better understanding and satisfaction.
By using a variety of different methods, physicians can effectively teach patients about their anatomy, reassuring and educating women about their bodies and progress of treatment. This engagement empowers patients to take an active role in the medical process, leading to more positive patient outcomes.
Learn more about how patient experience impacts health outcomes>>







